The OCD cycle is fueled by intense anxiety as well as an overwhelming desire to find relief.
You’re driving along your usual route home from work when you hit a little bump. What was that? You look in your rear view mirror but don’t see anything. You try to keep driving along, but your anxiety increases. It continues to climb until it’s unbearable.
You finally give in to your anxiety and turn around. You just need to double check to make sure you didn’t hit an animal or a person. You circle around and around until your anxiety decreases.
This is the OCD cycle.
Obsessive-compulsive disorder (OCD) is a mental health condition characterized by a cycle of obsessions and compulsions.
Obsessions are persistent and intrusive thoughts, images, or urges that trigger intense anxiety. Regardless of the focus, all OCD obsessions have a few things in common: They are unwanted, repetitive, and distressing.
Compulsions are the behaviors (external actions or internal thoughts) you perform in an attempt to get rid of the unwanted thoughts and feelings. Compulsions are fueled by an intense desire to reduce your fear and anxiety.
For instance, if every time you drove over a pothole, you believed you had run over a person or animal, this would be considered an obsession. Turning around and driving back to the pothole (perhaps even several times) to ensure you hadn’t hit anything would be the compulsion.
OCD can significantly affect your daily life. An OCD diagnosis means you spend at least
OCD is often referred to as a “vicious” cycle because the obsessions and compulsions happen in a loop that can be extremely challenging to break. The longer you remain in the cycle, the more momentum and strength it gains, making it even more difficult to escape.
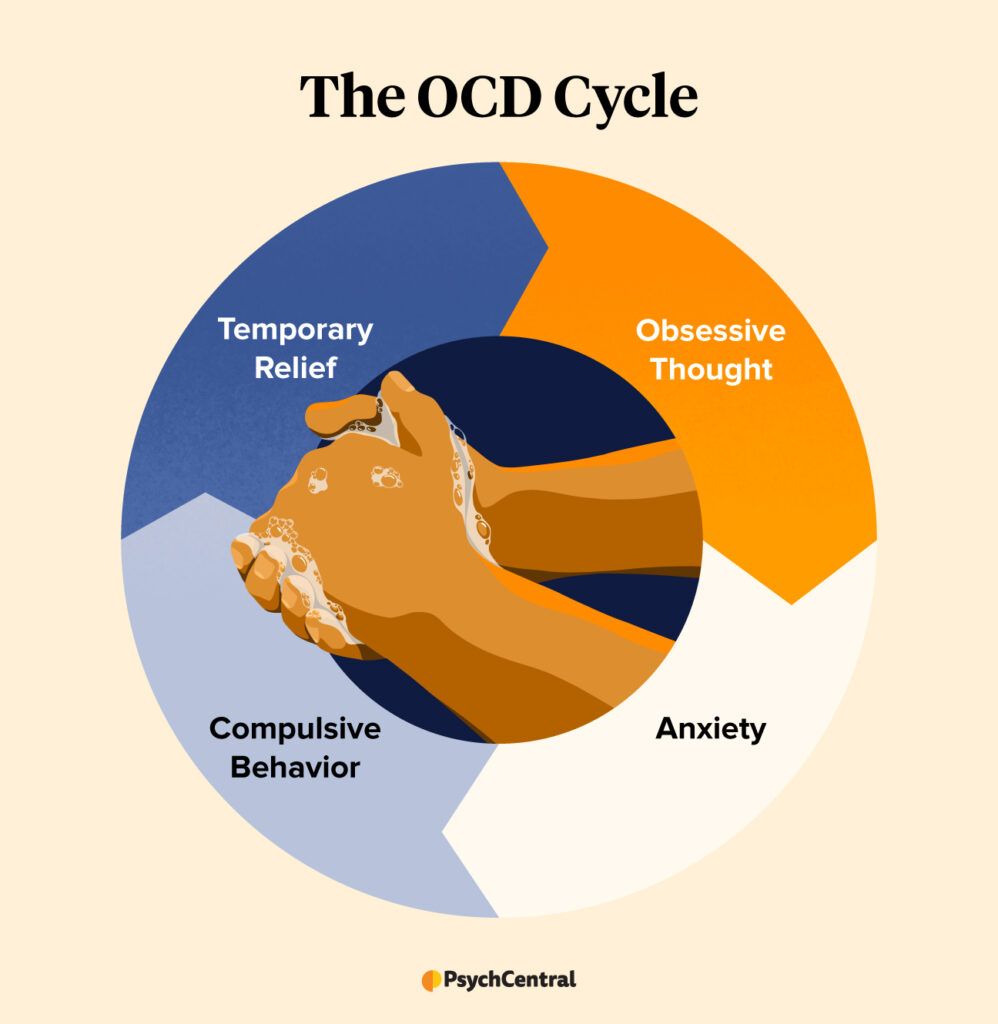
The four stages of the OCD cycle include:
- obsessions
- anxiety
- compulsions
- temporary relief
Obsessions
OCD obsessions vary widely from person to person and may revolve around any topic you can imagine. Some of the most common types of obsessions include thoughts about germs, religion, sexuality, magical thinking, or violence.
Obsessions can be distressing and ego-dystonic, meaning they don’t align with your beliefs or self-concept. They can be particularly distressing if you give them significant meaning or have low levels of insight.
According to the Diagnostic and Statistical Manual of Mental Disorders, 5th edition (DSM-5), OCD insight may be
- Good or fair insight. You acknowledge that your OCD thoughts are definitely or probably not true.
- Poor insight. You think your OCD thoughts are probably true.
- Absent insight/delusional beliefs. You are completely convinced that your OCD beliefs are true.
Research shows that poor insight is linked to more severe and more complex symptoms and worse outcomes.
Anxiety
As would be expected, the highly distressing OCD obsessions cause significant levels of anxiety and fear. In fact, for several decades, OCD was categorized as an anxiety disorder in the Diagnostic and Statistical Manual of Mental Disorders.
People with OCD often misinterpret the high levels of anxiety to mean that something really bad is happening. This further plays into the idea that the thought is real. Then, in an attempt to reduce the crippling anxiety and fear, you feel compelled to perform compulsions.
Compulsions
Compulsions are the rituals you perform in an attempt to get rid of the distressing feelings of anxiety. These can be external behaviors or internal thoughts.
For instance, let’s say that you have an obsession that your mind can cause a natural disaster like an earthquake or hurricane. This thought is typical of “magical thinking” OCD, where you believe your thoughts can cause bad things to happen.
In this case, the compulsion might be that you have to mentally “cross out” the thought 100 times to keep everyone safe.
Temporary relief
Once you’ve finished your compulsions, you might feel OK for a little while. The calmer feeling won’t last long, however, as OCD has a way of continuously creating more obsessions.
The entire cycle will continue to repeat itself as long as you fear and resist the obsessions.
The OCD cycle is fueled by high levels of anxiety and fear, as well as an intense desire to reduce that fear.
Though it sounds counter-intuitive, experts recommend that you practice accepting your thoughts and refrain from carrying out your compulsions. This is the basis of exposure and response prevention (ERP) therapy.
If you’re able to “surrender” and accept the “worst case scenario,” it prompts your natural thoughts and feelings to come back. This trains your brain to recognize that your OCD isn’t so scary after all.
There are several things you can do to help break the OCD cycle, including medication and therapy, as well as everyday strategies.
- Exposure and response prevention (ERP). This is the first-line therapy for OCD. ERP gradually exposes you to your OCD fear until you’re no longer afraid. About
80% of clients with OCD respond well to ERP.
- Be willing to accept uncertainty. OCD can make you feel desperate to know certain things, including whether you harmed someone or if a particular type of shampoo can cause cancer. Try to say to yourself, “maybe, maybe not,” and let it go as best you can.
- Avoid seeking reassurance. Seeking reassurance is a type of compulsion. For instance, you might worry that you hit a cat while driving simply because you felt a bump, and the fear overwhelms you. Try your best not to drive back out and look for the cat.
- Mindfulness meditation. Practicing mindfulness is a long-term strategy, as it slowly reduces your overall anxiety levels. One
study shows that mindfulness-based cognitive strategies can reduce harmful OCD beliefs and act as an effective therapy alongside ERP.
- Medication. Antidepressant medications, such as selective serotonin reuptake inhibitors (SSRIs) and clomipramine (tricyclic), are the first-line medications for OCD.
The OCD cycle consists of 4 basic parts: obsessions, anxiety, compulsions, and temporary relief. It’s considered a “vicious” cycle because once you get pulled into it, it gains momentum and strength, making it even more difficult for you to get out.
The best way to put an end to the cycle is to practice exposure and response prevention. This means you “accept” the thoughts, live with the uncertainty, and refrain from engaging in compulsions.
If you or a loved one lives with OCD, don’t hesitate to reach out to a mental health professional to discuss your treatment options.
